How to CBRN-proof Your Hospital
Ioannis Galatas1
1 International CBRNE Institute, Charleroi, Belgium
Introduction
One day an improvised explosive device was detonated in a busy district downtown in a Western capital. Ordinary first responders (policemen, firemen, ambulance service crews) were deployed to secure the area, collect evidence, and transfer casualties to one or more hospitals close to the incidence site. One hour after the explosion, one of the firemen decided to try the new chemical and radiological detection equipment his/her service recently purchased. For his/her surprise the detector started beeping indicating the presence of radiation (dirty bomb or radiological dispersal device – RDD) – alternative scenario: the chemical detector was activated (chemical bomb or chemical dispersal device). He/she immediately informed own headquarters in order certain actions to be taken. In the meantime, casualties arrived at the emergency department of the hospital(s); some met with relatives; others underwent emergency surgery; other underwent CT scans or x-rays while most of them came into close contact with emergency department’s personnel. All these people were unaware of the fact that casualties were not only wounded but contaminated as well. This is not a science fiction scenario but one that might happen tomorrow somewhere. No matter when or where, casualties/patients/victims all end up to hospitals that have to be prepared to deal with both conventional and asymmetric threats.
Against this possibility comes the inherent attitude that such a combination is too exotic to happen in a specific city or in a specific hospital. The second universal objection is the budget reduction that affects hospitals as well thus making purchase of specialized equipment more difficult than ever. Third, it is the perception of the people involved in hospital’s defense. The same people – physicians and nurses – who have to safeguard the hospital in order to avoid secondary contamination, need to spend a lot of time and effort in the theoretical study and practical training that will make them proficient in receiving contaminated casualties. As a matter of fact, this is a separate medical specialty that includes elements of many other sciences (i.e. chemistry, physics, radiation, epidemiology etc.) totally different than their current medical specialty and without any immediate personal compensation or something to add to their curriculum vitae. Finally, it is the state that shares all the above negative attitudes and does not create and impose a common unified chemical, biological, radiological, nuclear and explosives’ (CBRNE) response and preparedness program that all hospitals must follow and comply with.
Studies from 2001 until 2017 highlight that the medical sector is the weakest link in all national CBRN emergency response plans (Table 1). If results shown are acceptable for the years 2001-2005, they are not acceptable for the last decade that CBRN threats have been stabilized in the first three ranks of threats’ estimates. It is of note that even when mega sports events were at streak (years: 2008-2012-2016), the preparedness level was still problematic despite the international reassurances given that the hosting nation was fully prepared to deal with this specific threat.
Table 1. Studies on medical sector’s CBRN preparedness from 2001 to 2017
2001
Treat K, et al (2001). Hospital Preparedness for Weapons of Mass Destruction Incidents: An Initial Assessment. AnnEmerg Med 38(5):562–565
Conclusion: Hospitals in this sample are not prepared to handle WMD events.
2002
George G, et al (2002). Facilities for Chemical Decontamination in Accident and Emergency Departments in the UK. Emerg Med J19:453-457
Conclusion: Most departments had some equipment for chemical decontamination. However, there were major inconsistencies in the range of equipment held and these limited its usefulness. Only a small minority of departments was satisfactorily equipped to deal with a serious chemical incident.
2006
Wong K, et al (2006). Preparation for the Next Major Incident: Are We Ready? Emerg Med J 23(9): 709–712.
Conclusion: Still considerable room for improvement in British hospitals’ readiness for a major incident. The situation has changed little since similar studies were done from 1994 to 2002. Urgent investment, education and rehearsal of Major Incident Plans is recommended.
2007
Ziegler A. Hospital Preparedness for Contaminated Patients in Austria. Presented at the 15th World Congress on Disaster and Emergency Medicine; 13-16 May 2007, Amsterdam, The Netherlands.
Conclusions (from118 acute care hospitals in Austria): Hospitals must NOT rely on on-site decon; Patients will surely bypass EMS; Well documented risks for hospitals include: secondary contamination of staff and disruption of hospital services; Hospital preparedness for contaminated patients is low; Decon facilities and PPE are absent in many hospitals; Contamination topic was included only in 1/3 of the plans; Ability to implement plans is doubtful; Contaminated-related training and exercises? The exception not the rule!; Awareness of PPE in hospitals is particularly low.
Williams J, Walter D, Challen K (2007). Preparedness of Emergency Departments in Northwest England for Managing Chemical Incidents: A Structured Interview Survey. BMC Emergency Medicine 7:20.
Conclusion: Major inconsistencies in the preparedness of North West Emergency Departments for managing chemical incidents. Nationally recognized standards on incident planning, facilities, equipment and procedures need to be agreed and implemented with adequate resources. Issues of environmental safety and patient dignity and comfort should also be addressed.
Anathallee M et al (2007). Emergency Departments (Eds) in the United Kingdom (UK) Are Not Prepared for Emerging Biological Threats and Bioterrorism. J Infection 54(1) 12-17.
Conclusion: EDs in the UK are not prepared for emerging biological threats and bioterrorism. With current facilities and procedures, it is highly likely that an infectious agent will spread to staff and other patients in any future biological incident.
2005-2008
ETHREAT Project (European Training for Health Professionals on Rapid Response to Health Threats)
Planning and developing an educational package incorporating the knowledge and training material necessary to empower European Front-Line Health Professionals, including armed forces health personnel, to rapidly, clinically recognise and adequately respond to modern public health threats, like attacks with Chemical, Biological and Radiological agent.
One of the questionnaires of this project addressed CBRN experts who were asked to comment on: “What proportion of FLHP in your country is adequately prepared to recognize and manage CBR threats”
http://euprojects.org/ethreat.info/
2010
Cole J (2010). UK Medical Responses to Terrorism. Chapter 9. In: Medical Response to Terror Threats. Ritchman A, et al (eds). IOS Press.
Conclusion: Robust emergency plans need to be in place and effective communication must be maintained throughout the incident – within organizations, between responder agencies and also between responding authorities and the affected public.
McLoughlin T.F (2010). Discussion Regarding CBRN Training for Emergency Room Staff. J Med CBR Def; Volume 8.25.
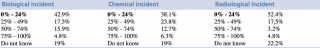
The duty charge nurses from every responding emergency department (31 out of a possible 46 ER departments in London responded, 67%) were asked “How often do key ER staff train for a CBRN incident?”
Results: The replies varied considerably and ranged from training weekly to once every 3 years at one department.
Conclusion: Given that 42% of units believe that key staff training is required twice a year anything less than this should be considered as being outside the norm and therefore unacceptable.
2011
Kollek D, Adam Cwinn A (2011). Hospital Emergency Readiness Overview Study. Prehospital Disaster Med 26(03):159-165
Conclusion: “… despite improvements, there remain gaps in Canadian healthcare facility readiness for disaster, specifically one involving contaminated patients.”
McInerney JE, Richter A (2011). Strengthening Hospital Preparedness for Chemical, Biological, Radiological, Nuclear, and Explosive Events: Clinicians’ Opinions Regarding Physician/Physician Assistant Response and Training. Am J Disaster Med 6(2):73-87.
Conclusion: Improving healthcare preparedness to respond to a terrorist or natural disaster requires increased efforts at organization, education and training. Physicians are willing to increase their knowledge base if it is possible to create a mutually positive win-win environment to minimize cost and disruption while maximizing preparedness. There is no clear consensus on the implementation of this training, but to most efficiently and effectively use scare homeland security dollars, a dialogue must begin between the medical profession, medical societies, and US Department of Health and Human Services to determine the best training strategies.
Ready or Not? Protecting the Public Health from Diseases, Disasters and Bioterrorism (2011). Trust for Americas Health.
Major ongoing gaps: … As baby boomers begin to retire, there is not a new generation of workers being trained to fill the void.
2012
Smith C, Hewison A (2012). Are Nurses Prepared to Respond to a Bioterrorist Attack: A Narrative Synthesis? J Adv Nursing 68(12):2597-2609.
Conclusion: Existing nurse education in areas such as infection control can incorporate bioterrorism training to improve preparedness, yet nurses must also prepare themselves personally for a bioterrorist attack.
Gursky E, Bice G (2012). Assessing a Decade of Public Health Preparedness: Progress on the Precipice? Biosecurity and Bioterrorism: Biodefense Strategy, Practice, and Science 10(1):55-65.
Conclusion: Currently, a rapidly diminishing public health infrastructure at the state and local levels as a result of federal budget cuts and a poor economy serve as significant barriers to sustaining these nascent federal public health preparedness efforts. Sustaining these improvements will require enhanced coordination, collaboration, and planning across the homeland security enterprise; an infusion of innovation and leadership; and sustained transformative investment for governmental public health.
Mérens A, et al (2012). Assessment of the Bio-Preparedness and of the Training of the French Hospital Laboratories in the Event of Biological Threat. Euro Surveill17(45): pii=20312.
Conclusion: The main lesson learnt in these 4 exercises was that the key to successful detection of biological agents in case of a biological threat was standardization and validation of the methods implemented by all the laboratories belonging to the network (“Biotox-Piratox”).
Dabrera G, et al (2012). Is Preparedness for CBRN Incidents Important to General Practitioners in East London? Journal of Business Continuity & Emergency Planning 6 (1):47-54.
Results: Of 157 GPs, 56 responded, although some responded collectively for their practice. The majority of respondents recognized roles for themselves in CBRN incidents, including recognition of illness, supporting decontamination, and appropriate reporting. However, 79% of GPs also felt unprepared for such incidents. The most popular topic for training to address this was clinical presentation of CBRN exposures. Most practices had no policy for dealing with suspect packages and white powder incidents. Since this survey, guidance and training has been made available to local GPs. As the UK will host more events like the 2012 Olympics, preparedness for GPs will continue to be an important consideration in the UK.
Mitchel C, Karmhan G, Higginson R (2012). Are Emergency Care Nurses Prepared for Chemical, Biological, Radiological, Nuclear or Explosive Incidents? Intern Emergency Nursing 20(3):151-161.
Conclusion: There is a need for a standardized ‘blueprint’ of role-specific competency criteria for a CBRNe incident for all emergency healthcare staff. The assessment tool used in this study can help to assess levels of preparedness amongst nursing staff and, if adapted accordingly, help gauge preparedness of other key healthcare professionals.
Galatas I (2012). 2012 Olympic Games – Terrorist CBRE Threat Estimate and Medical Response. Int J Emergency Management 8(3):228-38.
2012 us the year of the Olympic Games that will be held in London, UK. This mega sport event is a terrorist challenge especially now that Osama bin Laden is dead and his successor is struggling to regain “face” amongst Islamic extremists opposing the West. New emerging threats such as CBRE agents’ release in urban/megapolis environment must be taken seriously and state response must be fortified against this visible possibility. Medical/hospital CBRE defense and preparedness is of mandatory importance because medical consequences might last for months or years. A terrorist CBRE threat estimate is provided along with an analysis of hospitals’ preparedness in order to assist first responders perform in a most effective way in order to minimize casualties and consequences. Following Japan’s triple catastrophe nobody has the right to consider CBRN release a science fiction. It might happen to us as well! Tomorrow!
2013
Hung KKC, et al (2013). Emergency Physicians’ Preparedness for CBRNE Incidents in Hong Kong. Hong Kong Journal of Emergency Medicine 20(2):90-97.
Conclusion: This study demonstrates ED doctors’ low confidence in managing specific CBRNE incidents. Current strengths identified include the good awareness of hospital emergency plans and high motivation to get more training.
2014
Mortelmans LJ, Van Boxstael S, De Cauwer HG,Sabbe MB (2014). Preparedness of Belgian Civil Hospitals for Chemical, Biological, Radiation, and Nuclear Incidents: Are We There Yet? Belgian Society of Emergency and Disaster Medicine (BeSEDiM) study. Eur J Emerg Med21(4):296-300.
Conclusion: There are serious gaps in hospital preparedness for CBRN incidents in Belgium. Lack of financial resources is a major obstacle in achieving sufficient preparedness.
Zaboli R, Sajadi HS (2014). Assessing Hospital Disaster Preparedness in Tehran: Lessons Learned on Disaster and Mass Casualty Management System. Int J Health System Disaster Management 2(4);220-24.
Conclusion: Hospital emergency incidence commanding systems is a standard system that can be used by all hospitals both in national and local levels. Using this system in hospitals, along with the systematic arrangement of human resources and exact distribution of managerial duties and developing a commanding unity can improve crisis management in hospitals.
2015
Jan Schumacher, et al (2015). Survey of UK Health Care First Responders’ Knowledge of Personal Protective Equipment Requirements. Prehospital Disaster Medicine 30(3):254-58.
A total of 98 specialist registrars (in Anesthesiology [n-51], in Emergency Medicine [n=21] and in Intensive Care Medicine [n=26]) completed hand-delivered surveys. The best knowledge of PPE requirements (76%) was found for acute respiratory syndrome (SARS), with less knowledge about PPE requirements for anthrax, plague, Ebola virus disease (EVD) and smallpox (60%). The results show limited knowledge of PPE requirements (20-30%) for various chemical warfare agents. Personal protective equipment knowledge regarding treatment of sarin-contaminated casualties was over-rated by 80% and for patients with EVD it was over-rated by up to 67% of participants.
Conclusion: The results of the tested cohort indicate that current knowledge regarding PPE for chemical warfare agents remains very limited.
Ingrassia P, Caviglia M,Djalali A (2015). Analysis of Risk Management Planning and Perception to Counter the Terrorist Threat within the Health Sector of European Union Critical Infrastructure Protection. Report No: DR/2/001. EU THREATS Project (Terrorist Attacks on Hospitals: Risk and Emergency Assessment, Tools & Systems).
Conclusions: In 70% of cases the hospital stockpiles PPE against CBRN (Chemical, biological, radiological and nuclear) threats, but only in half of the cases the hospital personnel, in particular staff of ED department, receive specific training in proper use of it; in addition, 61% of the hospitals are also equipped with decontamination facilities. The main barriers to crisis management capability seems to be financial shortcoming (68%), followed by low priority (59%) and poor knowledge and competencies of personnel (51%).
2016
Jama T, Kuisma M (2016). Preparedness of Finnish Emergency Medical Services for Chemical Emergencies. Prehospital Disaster Medicine 31(4):392-396.
Conclusions: Emergency Medical Services capacity in Finland for treating chemically affected patients in the field needs to be improved, especially in terms of antidote therapy. Mobile decontamination units should be available in all hospital districts.
2017
Olivieri Carlo, et al (2017). Hospital Preparedness and Response in CBRN Emergencies: TIER Assessment Tool. Eur J Emergency Medicine 24(5):366–370.
Conclusion: Hospitals need a specific level of preparedness to enable an effective response to CBRN emergencies. The assessment tool, developed through experts’ consensus in this study, provides a standardized method for the evaluation of hospital preparedness and response performance with respect to CBRN emergencies. The feasibility and reliability of this assessment tool could be evaluated before and during simulated exercises in a standardized manner.
Mortelmans LJM, et al (2017). Are Dutch Hospitals Prepared for Chemical, Biological, or Radionuclear Incidents? A Survey Study. Prehosp Disaster Med32(5):1-9.
Conclusion: There is a serious lack of hospital preparedness for CBRN incidents in the Netherlands.
Al-Shareef AS, et al (2017). Evaluation of Hospitals’ Disaster Preparedness Plans in the Holy City of Makkah (Mecca): A Cross-Sectional Observation Study. Prehosp Disaster Med32(1):33–45.
Conclusion: This study demonstrated that there is significant room for improvement in most aspects of hospital Emergency Operations Plans, in particular: reviewing the plan and increasing the frequency of multi-agency and multi-hospital drills. Preparedness for terrorism utilizing chemical, biologic, radiation, nuclear, explosion (CBRNE) and infectious diseases was found to be sub-optimal and should be assessed further.
Despite existing problems all medical people involved in hospitals’ preparedness must realize that the threat is real and following the recent and ongoing shrinking of the Islamic State and the influx of foreign fighters back to their homelands (mainly in Europe) many of which have combat experience and certain dexterities in explosives and chemicals, the possibility of a chemical or radiological terrorist incident is not futuristic anymore and should be adequately prepared to avoid being sorry for themselves and their patients.
There are certain things that need to be addressed and certain solutions or proposals to be taken care of that will fortify hospitals and minimize the consequences.
Architecture and geography
As a principle, in modern hospitals the outdoor environment is usually composed by vast gardens and green fields that soothe the sick and support their fast recovery. But how can the hospital control the incoming contaminated flow of victims rushing to the nearest hospital without a solid hard fence and a strong gate? Ground floor has tens of doors and windows that can provide entry to hospital if unguarded, unlock or easy to brake by frustrated incomers in need. Their uncontrolled entry will lead to overall hospital’s secondary contamination and make things worse. In that respect, hard perimeter fence; main gate; secure/locked ground doors and windows are mandatory precautions to preserve hospital’s integrity and working personnel’s safety. Addition of a fence is costly and hardening of doors and windows with special films might be expensive as well. In contrast, most military hospitals are considered as military camps and do have a high perimeter fence and a main gate with a post.
The distance of a hospital from potential targets is of significant importance because it defines the response time of the involved entities. For example, a hospital located near a major subway station might have zero or near-zero response time; a hospital located far from targets might have more time to organize its response but due to distance only few victims will go there even if it is a CBRN specialized hospital. The Tokyo sarin incident (1995) dictates that all hospitals and clinics in a (at least) major city should be prepared to accept contaminated casualties – 169 Tokyo medical facilities were involved in the management of casualties and worried well citizens.1
Security personnel
All hospitals have them and they are very important for the daily function of the hospital (incoming vehicles and visitors, wards’ security, implementing the visiting hours’ program etc.). But can the hospital count on them for controlling the incoming flow of contaminated victims without specialized training, specialized equipment, and hands-on experience? Surely not! Most probably they will either lock themselves inside hospital or leave premises. Situation might be better in the military hospitals but even there training and equipment needs to be available and know how to use them. Specialized equipment and training cost money as well.
Planning
Plan is nothing; planning is everything! In that respect hospital needs to have a small, flexible, realistic, updated and anthropocentric plan readily available to all those involved. Planners’ worldwide need to answer a very simple question: “What would be my reaction, if I was involved in a real CBRN incident?” Planners’ should plan based on what people will actually do; not on ideal responses and academic expectations that usually have no place in actual mass emergency situations. Thus the anthropocentric (from Greek: anthropos [man] + kentro [center]) element should be prominent and the most important pylon in planning process. Plans do not cost a lot but require a lot of brain work and hands-on operational experience! A plan also reveals the background of a planner. It is very obvious that the planner has never been to a personal protective equipment (PPE) ever in his/her life when reading that first responders donned in Level-A PPE will do everything inside the Hot Zone – from sampling and detection to carrying stretchers with victims!
Exercises and drills
The best way to test plans and preparedness is by conducting exercises and drills. Although all know that this is true usually either they do not do it or do it wrong! One big CBRN drill every two years equals nothing! One pre-scheduled drill is best for policy/publicity reasons but operationally equals nothing as well! Because in real life an incident will happen right here, right now! Usually bad things happen during off-working hours, vacations and holidays or weekends or during the night. In that respect exercises and drills within the hospital or with neighboring hospitals both at local and national levels should take these elements into account in order to generate drills that will stimulate personnel and simulate reality as close as possible. Exercises and drills do not stop at the entrance of the hospital or when casualties are safe inside ambulances. Ask your ambulance crews to proceed to the nearest hospital and deliver their casualties to the Emergency Department (ED) without a notice. This might change your preparedness mindset completely. Continuous acclimatization to PPE is mandatory and should be incorporated in each department’s routine activities. Wearing PPE once or twice a year, it would be like the first time! Medical interventions while in PPE requires a lot of training to overcome the reduced dexterity of thick rubber gloves.
Hospital’s personnel
This is the key player in all response plans worldwide. Without them no plan is effective or applicable. All should be involved at various levels of engagement. All should be educated and trained depending on their specialty and duties assigned with special emphasis to ED’s personnel but also to certain medical specialties closely related to CBRN agents (i.e. chest physicians; ophthalmologists; pediatricians; dermatologists, etc.). If they are not very enthusiastic about their involvement, speak with them to dig out why and improvise ways to motivate them. CBRN medicine is kind of a medical specialty requiring a lot of studying, training in difficult environments, performing duties while wearing uncomfortable PPE compromising senses and dexterities – and all that for what? Just for an incident once in a life time; if ever? At the same time, they have to face their daily emergencies, to take care of their patients, to improvise based on their deep medical knowledge and lots more. On top of these, we ask them to add another specialty as described above? These are only few of the questions and doubts posed to and by medical personnel. Think of intelligent approaches for intelligent people, fight their fears generated by ignorance, and infuse interest through modern educational methodologies – you might be surprised by their reactions and change of overall attitude. If we ever manage to introduce “CBRN Medicine” into the curricula of the medical and nursing university schools this would be the first step towards better educated future front-line health professionals that one day might be confronted with the real enemy. And this does not cost a lot!
Infrastructure
a. Decontamination facilities look expensive but are they? Depending on the hospital’s budget and strategic mission there are many commercial solutions available in two forms: deployable and fixed. The first choice is usually a trailer containing deflated tents and related decontamination equipment. The latter is a separate/adjacent infrastructure (usually four rooms) that serves the purpose. The ideal setting is to have an ED with two separate entrances: one leading to “regular” ED for daily emergencies and the other (CBRN/HAZMAT [HAZardousMATerials), leading to a decontamination station connected to the regular ED. In case of an emergency – especially if the incident’s scene is in close proximity to the hospital and response time is almost zero – hospital seals the one door, opens the CBRN/HAZMAT entrance, and is ready for accepting contaminated casualties. All the above raise an important issue that usually is not taken into account. It is cheaper if we incorporate decontamination facilities and capabilities during the hospital’s design phase instead of hardening premises later on under the pressure of change of threat estimate. A good solution for this is to put the civil engineers/architects’ community into contact with medical/health community and CBRN experts. Collaboration will surely provide clever and affordable solutions. On the other hand, what is the difference of a fixed or deployable decontamination system with the showers we have at home? Improvisation will save money and will come up with custom-made solutions that fit specific needs. Imagine placing a big number of showers on the perimeter ground walls of a hospital; then connect them with the main water supply system, install a waste water collection tank underneath, add a number of privacy panels and you are set to go with a fraction of money. Use pipes, nuzzles, and hoses and you can construct your own decontamination systems for your first responders as well! Fixed decontamination stations might look very expensive but the overall cost to benefit ratio is quite attractive in the long run.
If the above are still expensive for you then close collaboration with your local fire station is a one-way solution. Firemen are very good in providing “water curtains” (high volume/low pressure [50-60psi]) at no time. But you have to test this solution and solve the small problems that come with it by working together with them and let them know what you want them to do.
Other issues of concern are the isolation rooms (with positive/negative pressure) and radiation rooms (for inner contaminated casualties especially following a RDD detonation).
b. Existing laboratories pose a second problem. Are they at least of bio-safety Level -2 (BSL-2) quality? Do they have any bio-safety lab Level-3 (BSL-3) capabilities or do you have to transfer samples to an authorized BSL-3 or BSL-4 lab? Is the reference lab within the country or need to send samples abroad? Does hospital lab have proper protocols and means for transferring highly contagious samples? Does it have the equipment for fast verification of exposure to chemical warfare agents (i.e. biomarkers for exposure to organophosphates)?
c. Field hospitals: Hospitals can easily handle big numbers of “clean” chemical casualties. But can they equally perform when confronting biological or radiological casualties? Are there any quarantine hospitals included in response plans? A field hospital (tents or containers) is a good solution and can be transported near to the infected area fulfilling the basic rule indicating that in biological attacks casualties are not transferred to hospitals; instead, hospitals are transferred to casualties. Armed Forces worldwide do have field hospitals for their own operational purposes – are these hospitals suitable to operate in a contaminated environment as well?
Equipment
Most of the equipment that hospital’s personnel will need is already available and used on routine basis (e.g. IV fluids, intubation sets, suction pumps, hemostatic tourniquets, consumables etc.). In addition to these, specialized items need to be purchased.
a. PPEs: Best choice for ED’s personnel is the powered air-purifying respirator (PAPR) ensemble that is comfortable and provides wide view helmet without restrictions on facial hair, glasses etc. In combination with a splash proof (water resistant) suit, makes an ideal ensample serving all purposes including decontamination procedures.
Biological threats (e.g. Ebola virus) need different PPEs for the protection of personnel involved. So far the related technical document produced by the European Center for Disease Control (ECDC) is highly recommended2 and so is the new PPE prototype MKVI proposed by John Hopkins University.3 Same applies for another ECDC technical report addressing the issue of aerial medical transportation of bio-contaminated patients.4 There are many related solutions in the market – choose one that can be folded (to save space) and can provide both positive and negative pressure inside the transportation capsule (it can be used for both biological and chemical/radiological agents’ exposures).
Radiological casualties represent another category we should also focus on mainly because our medical knowledge on management issues is rather limited. Even specialists in nuclear medicine and medical physics are not very familiar with triage and management protocols in case of mass casualties following a RDD’s detonation in urban environment. An excellent source of related information is the Radiation Emergency Medical Management (REMM) website5 that is highly recommended for further exploitation and study.
b. AMBU and ventilators: Since the area outside the ED is considered a “warm zone” (contaminated) it is best to use equipment connected with gas filters (like those used in gas masks – i.e. AMBUMilitaryMark III resuscitator or Pneupac/ParaPAC ventilator).
c. Field consumables: There are only three medical interventions that can be performed under PPE in a contaminated environment: provide auto-injectable antidotes (for nerve gases and cyanide); support respiration (chest seals would be beneficial in case of an explosion) and control hemorrhage (with modern hemostatic sponges or gauges). Remember: it is important to keep contaminated casualties alive until they are “clean” (decontaminated) and ready to undergo a proper triage at the ED where all means would be available to support their survival.
Interoperability and compatibility
These are two terms that the military love the most but civilian counterparts usually forget their importance. Imagine two hospitals having two different decontamination systems – one has it in deflated tents and the other in a container: what will actually happen when one hospital will be asked to support the other? Upon arrival, personnel of the first hospital will found themselves in an unfamiliar working environment and in the middle of havoc you do not ask questions or read the operational manual! Imagine now that these two hospitals had the same field equipment: upon arrival, the new crews will immediately start providing services by using their “own” systems. Sounds simple and logic but these are two qualities often forgotten or neglected during planning phases! Unfortunately, quite often, military hospitals ignore these terms as well not to mention that the civilian-military hospital collaboration is not always ideal.
Morgues and contaminated corps’ management
Hospitals are not equipped to handle big numbers of corps nor contaminated corps. In that respect hospitals need to have solutions ready and applicable that will provide the time required for the adequate management of this problem. Cemeteries might have big refrigerated rooms that can be used; commercial refrigerated trucks can be deployed provided that you remove all identification markings from outside surfaces; ice-skating halls might provide more space for storing the dead as well. The huge morgue facility deployed within 72 hours after the 7/7 London bombings (2005) represent a fine example of a holistic solution with excellent working environment and consideration of many ethical issues derived from the multiculturalism of the victims.6 Take also into consideration the burial processes to be used for the various types of CBRN contamination. This is one of the major problems communities affected by the ongoing Ebola outbreak in certain African countries: superficial burial led to secondary infection of stray carnivores digging into the shallow graves looking for food.7,8
In conclusion
The topic is complex and multi-dimensional and this article addresses only the headlines of hospitals’ CBRN defense and preparedness. Deeper study and thorough evaluation is needed for a successful outcome. But even the summarized information provided herein should be enough to alert hospitals’ civilian and military officials on their potential to deal with asymmetric threats producing mass casualties in urban environment while providing two alternatives: to pray nothing that horrible ever happens in their city or to do something to protect both their hospital and people working therein. It is their choice and so are the consequences of their decisions! Open source intelligence reveals that the Islamic State has chemical and radiological terrorist ambitions and their immoral barbaric behavioral modus operandi reveals that they are capable of releasing CBRN agents against Western infidels.
In conclusion there are some key points that need to be taken into serious account in case authorized personnel decides to step up and take actions:
- Anthropocentric planning is mandatory;
- Save the savers/first receivers to save the hospital;
- Continuous exercising and acclimatization to PPE is the antidote against fear and ignorance;
- HAZMAT/CBRN treatment is mostly empirical and requires a lot of studying and field improvisation;
- All medical specialties will be involved;
- Medical decisions might contradict ordinary medical ethics and regulations;
- Interoperability of modus operandi and compatibility of equipment are important elements in CBRN planning;
- Introduce “HAZMAT/CBRN Medicine” to medical schools’ curricula – invest in the future!
References
- Ortatatli M and Kenar L. Role of Military Hospitals in Handling Chemical and Biological Casualties. In: Arora R and Arora P (eds). Disaster Management: Medical Preparedness, Response and Homeland Security. CAB International, p.287. doi: 10.1079/9781845939298.0000
- ECDC (2014): Critical Aspects of the Safe Use of Personal Protective Equipment. Version 2: December 2, 2014. http://ecdc.europa.eu/en/publications/Publications/safe-use-of-ppe.pdf
- Johns Hopkins Personal Protective Equipment Prototype for Ebola (2014). https://www.youtube.com/watch?v=kRab2bGahCE
- ECDC (2014): Assessing and Planning Medical Evacuation Flights to Europe for Patients with Ebola Virus Disease and People Exposed to Ebola. October 21, 2014. http://ecdc.europa.eu/en/publications/Publications/ebola-guidance-air-transport-update-decontamination.pdf
- Radiation Emergency Medical Management (REMM). http://www.remm.nlm.gov
- Milton S (2006). Case Study – Honourable Artillery Company (HAC) Emergency Mortuary Facility, London. De Boer. http://www.deboer.com/_upload/documents/UK/Brochures/Case%20Studies%20-%20HAC.pdf
- World Health Organization (2014). New WHO Safe and Dignified Burial Protocol – Key to Reducing Ebola Transmission. November 7, 2014. http://www.who.int/mediacentre/news/notes/2014/ebola-burial-protocol/en/
- World Health Organization (2014). WHO: How to Conduct Safe and Dignified Burial of a Patient Who Has Died from Suspected or Confirmed Ebola Virus Disease. October 2014.http://apps.who.int/iris/bitstream/10665/137379/1/WHO_EVD_GUIDANCE_Burials_14.2_eng.pdf?ua=1